Every denied claim costs your practice time and money. When the CO-4 denial code appears on an Explanation of Benefits (EOB), it signals one specific problem. A modifier inconsistency, a missing required modifier, or documentation that does not support the modifier used.
According to AMA (American Medical Association) CPT guidelines, modifier errors rank among the top causes of claim rejections nationwide. For billing teams, unresolved CO-4 denials directly damage revenue cycle performance.
The CO-4 denial code falls under the Claim Adjustment Reason Code (CARC) system, maintained by the National Uniform Claim Committee (NUCC). Its official description states:
“The procedure code is inconsistent with the modifier used, or a required modifier is missing.”
In simple terms, the payer rejected the claim because the modifier attached to a CPT code does not align with billing rules, or the required modifier was completely absent.
CO-4 is a technical denial, not a coverage denial. The service may be fully covered. The problem is always on the billing side, which means it is fully fixable.
Note: Denial codes such as CO-4 are typically reported on the payer’s Electronic Remittance Advice (ERA), which explains why a claim was denied or adjusted. The ERA provides details about issues like incorrect coding, missing modifiers, or documentation errors. To understand how these reports work in the billing process, read our guide on “What Is ERA in Medical Billing.”
CO-4 often appears in remittance advice in one of three ways:
This is a compliance risk that goes beyond simple coding errors.
1. Missing Required Modifier
Certain CPT codes cannot be processed without a specific modifier.
2. Modifier-CPT Code Mismatch
Not every modifier pairs with every procedure code.
All creates direct conflicts that payers flag immediately.
3. Payer-Specific Modifier Rules
Applying uniform modifier rules across all payers is one of the most common and costly billing mistakes.
4. ICD-10 and CPT Pairing Issues
The diagnosis code must support the modifier used.

Many billing teams default to modifier 59 (distinct procedural service) when unbundling procedure pairs. However, CMS and a growing number of commercial payers now prefer, and in many cases require, the more specific X-modifiers in place of 59.
The four X-modifiers each carry a precise meaning.
Tip:
Using modifier 59 where an X-modifier is required may trigger CO-4. Review CMS NCCI guidance annually.
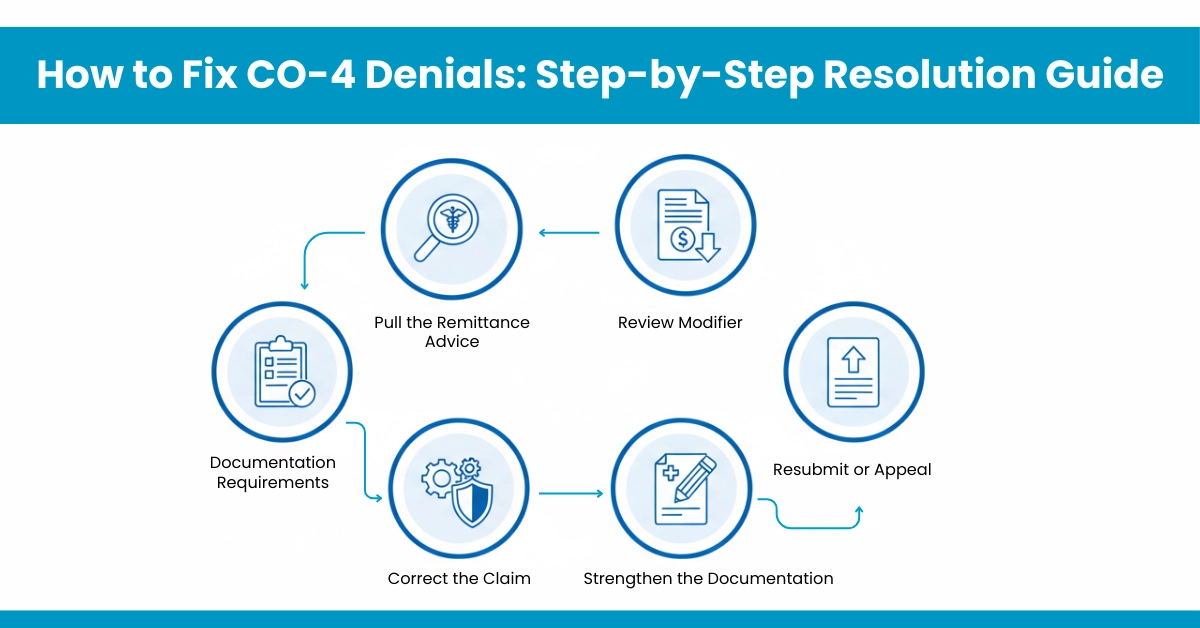
Prevention consistently saves more revenue than resolution.
The CO-4 denial code is one of the most preventable denials in medical billing. It always signals a modifier problem, either missing or inconsistent, that blocks payment unnecessarily.
Resolving denial code CO-4 requires accurate modifier knowledge, payer-specific awareness, and a structured appeal process. Preventing it requires proactive audits, updated coder training, and systematic denial tracking.
Practices that treat CO-4 seriously improve first-pass claim acceptance rates and recover revenue that would otherwise be permanently lost. If CO-4 denials are consistently impacting your revenue cycle, HelloMDs provides expert denial management, medical billing and coding, and full RCM healthcare services, built to reduce denials and protect your bottom line.
Follow Hello MDs on Facebook and Instagram to learn more about how our nationwide billing team supports your practice.
Disclaimer
The information provided in this article is for educational and informational purposes only and is not legal, medical, or financial advice. Practices and policies may vary by payer, region, and healthcare provider. Hello MDs certified medical billing professionals, follow these guidelines to manage claims accurately. Some images in this article are AI-generated for illustration purposes only.
Yes. Chiropractic billing uses unique CPT codes (98940–98942), specific coverage rules, Medicare restrictions, spinal manipulation documentation, and required modifiers, which differ significantly from physical therapy billing practices.
No. E/M codes are only billable when a significant, separately identifiable evaluation beyond routine chiropractic manipulation occurs, and it must be fully documented in the patient record.
Medicare requires SOAP notes, a documented subluxation diagnosis, a treatment plan, progress notes, and the AT modifier to prove active, corrective care instead of maintenance therapy.
Electronic claims are typically processed in 14–30 days, while paper claims may take 30–45 days. Payment timing depends on claim accuracy and individual payer processing rules.
Denied claims can be corrected, resubmitted, or appealed. Common resolutions include adding missing modifiers, correcting diagnosis codes, or improving documentation to meet payer requirements.